
This is “Chase”, who was one of my very special patients with GRPU that I will never forget. This article is dedicated in memory of Chase, and for all of my other patients with GRPU.
Terri L McCalla DVM MS DACVO
Did you know that there is a significant risk that your Golden Retriever will become blind in its senior years from a genetic disease lurking in its eyes? And that if you take action now, there is also a good chance that you can prevent your dog from going blind? This alarming disease is called Golden Retriever Pigmentary Uveitis (GRPU), and it is spreading by leaps and bounds, with the worst-affected dogs often ending up having both eyes removed. This is a fate that I hope that I can help your Golden avoid.
The three top genetic eye diseases in Goldens are cataracts , Progressive Retinal Atrophy (PRA) , and GRPU. But the worst of the three, and the most common, is GRPU. This disease also goes by the names Golden Retriever Uveitis, and also Pigmentary Uveitis; the most recently embraced term, however, is GRPU.
“Uveitis” is intraocular inflammation. Similar to “arthritis” (intra-articular inflammation), “uveitis” is an easier term to say. And just as arthritis can be caused by many things, so can uveitis. The hallmarks of ‘generic’ uveitis in an eye are redness of the conjunctiva, color change to the iris, squinting, pupil constriction/abnormal pupil shape, light sensitivity (photophobia), cloudiness of the eye, and low intraocular pressures. Some of these clinical signs are present in dogs with GRPU.
This article is a comprehensive go-to source for both owners and for general practice veterinarians (GPDVMs). Most GPDVMs have never heard of the disease, or if they have, their knowledge is scant. This is because there is very little written about the condition (see References ), and the available information is largely in specialty journals that GPDVMs would not have easy access to. I have attempted to provide all of the need-to-know information re: our current understanding of GRPU. Out of necessity, some of the information presented here is a summary of the author’s 20+ years of clinical experience treating dogs with GRPU, and thus is inherently biased.
GRPU must be properly diagnosed by Veterinary Ophthalmologists—it is not a disease that GPDVMs can accurately diagnose.
In the early 1990’s, veterinary ophthalmologists (VOs) in the Northeastern United States started to see a new eye disease that only affected Golden Retrievers. Dogs (most typically 8–9 years of age, but dogs as young as 2 years and as old as 13 years have been diagnosed with GRPU) were presenting with cloudy red eyes (usually both eyes) and varying degrees of vision loss. Many dogs had glaucoma (increased intraocular pressure= IOP) and/or cataracts. Vision loss was usually due to glaucoma.
Most affected dogs were not showing obvious signs of discomfort—they were just not seeing well (or at all). Sadly, however, they actually were uncomfortable (they had migraine-like pain from the glaucoma) but were not obviously showing it. Nothing could be done for the blind dogs to help them see again.
Then over the years, the disease spread to other parts of the country and GRPU became a common condition (especially the Pacific Northwest).
Fast-forward 20 + years: GRPU is the scourge of Golden Retrievers, and (in the author’s opinion) is the leading cause of blindness in this breed in the United States.
A landmark article about GRPU was published in 2000 in which the authors theorized that the disease is a genetic primary uveitis¹ (Note: this article is provided courtesy of Dr. John Sapienza). The mode of inheritance is unknown, but suspected to be either autosomal dominant with incomplete penetrance, or autosomal recessive. There is no sex predilection, and only the eyes are affected. Investigation of pedigrees revealed a common ancestry, as many Goldens in the Northeastern US have arisen from one common breeding stock. 1
Groundbreaking GRPU research at Purdue University College of Veterinary Medicine is performed by Dr. Wendy Townsend, who is a veterinary ophthalmologist. This research, both complex and time-consuming, is concentrated on identifying genetic markers which could then be used to develop a DNA test for GRPU.
As you are reading this, GRPU is spreading across the U.S and probably across the globe. The prevalence of the disease is difficult to pinpoint, as it is a moving target.
GRPU readily spreads because:
The prevalence of GRPU is not well known. However, a recent study of GRPU in three Midwestern states revealed a prevalence of 5.5% in all Golden Retrievers examined by a veterinary ophthalmologist; indeed, in dogs examined that were at least 8 years of age, the prevalence was 9.9%. 2 In other words, nearly 10% of all Goldens at least 8 years of age were found to be affected with GRPU. This is a very high incidence!
CERF data (genetic eye screening) of Golden Retrievers examined 2000-2008 yielded a diagnosis of GRPU in 0.2% of dogs examined; in 2009, 1.5% of dogs examined were diagnosed with GRPU. 2 Compared with the report of 9.9% incidence, these numbers are low. However, keep in mind that dogs submitted for CERF and OFA ECR exams are NOT the average Golden Retriever—they are generally high-quality younger breeding and/or show animals, and do not reflect the general pet population. OFA ECR examinations in the Pacific Northwest in one private referral practice have yielded a GRPU incidence of 25% – 33% in dogs 4 years of age and greater. 3 Additionally, in my private referral practice in the Pacific Northwest, approximately 36% of Golden Retrievers presented for an eye problem (not including OFA ECR exams) have been diagnosed with GRPU. These dogs are mostly family pets and not showdogs or breeding dogs.
NOTE: Just as with other dog breeds, it must be understood that many Golden Retriever breeders are not professional breeders. If dogs are bred by nonprofessional breeders, these animals usually do not have annual (or any) OFA ECR examinations. (AND—if your dog is AKC-registered, this does not guarantee anything regarding its health!) If you have a Golden Retriever as a family pet, do not assume that the breeder of your dog had annual OFA ECR examinations done on the parents or other related dogs. A professional breeder likely would have done so, and as proof it is routine for breeders to provide photocopies of both parents’ most recent OFA ECR exam results; these exams should have been done within one year of the breeding of the parents.
A limiting factor of OFA ECR exams is the availability of board-certified veterinary ophthalmologists to perform these exams; the ACVO (American College of Veterinary Ophthalmologists) provides a search function to locate ophthalmologists .
In order to understand the clinical signs, it is important to understand eye anatomy; please refer to this diagram . Note: The Anterior Chamber is not specified in the diagram; it is the dome-shaped, fluid-filled space between the cornea (the ‘clear windshield’ part of the eye) and the iris.
Typically, dogs are presented in crisis to veterinary ophthalmologists in the late stage of GRPU at 8 + years of age, with an average age of 8 to 10 years. “Crisis” means recent vision loss or reduced vision, accompanied by cloudy and/or red eyes. From the owner’s perspective, these clinical signs developed quite recently. However, from the veterinary ophthalmologist’s perspective, the clinical signs had been “brewing” for years, and only recently were they severe enough that the owner noticed a problem. This is very sad, because if these dogs had been examined annually by an ophthalmologist, GRPU could have been detected much earlier, the dogs then placed on lifetime medication, and vision likely saved.
Both eyes are almost always affected. The cause of impaired vision/blindness is usually glaucoma (increased intraocular pressure), but other conditions, such as cataracts and/or intraocular hemorrhage, can impair vision. If GRPU is too advanced and the eye(s) are blinded by glaucoma, vision cannot be recovered; sadly, in these cases both eyes usually need to be removed.
In retrospect, many dogs presented in crisis have a history of intermittently red/inflamed eyes that goes back several years. This redness is often mistakenly attributed to allergies (allergic conjunctivitis), and it usually temporarily resolves with topical steroid ophthalmic medication until the next episode of redness occurs. There is rarely any history of ocular discomfort or vision loss until the time of crisis. Sometimes there is a history of gradual cloudiness occurring, but usually owners will not present the dog to their family veterinarian for examination because the dog is comfortable and (apparently) seeing well. It is important to understand that affected dogs do not ‘complain’ or show outward signs that anything is wrong, until their vision declines.
Another clinical sign that is often present in affected dogs is iris cysts (also called ‘uveal cysts’). In a recent study, 34.8% of Golden Retrievers had iris cysts. 2 This is a very high incidence! Sometimes iris cysts are the first clinical sign noted by the family veterinarian (but it would be very easy for a GPDVM to not detect the presence of iris cysts). Not all dogs with iris cysts will develop GRPU, and not all dogs with GRPU have iris cysts. However, if either eye has iris cysts, this is a “red flag” and a risk factor for GRPU in a dog.
Iris cysts are fluid-filled membranes that form as “blisters” on the backside of the iris and/or ciliary body. They can range from light to dark brown, and when a beam of light is directed on them, it passes through the cysts (transillumination). The light brown cysts can be ghostlike and nearly completely transparent, making them very hard to detect. Iris cysts can “pinch off” and become free-floating little brown balloons inside the anterior chamber, or they can remain attached to the ciliary body and iris; the latter type are called iridociliary cysts and these are the typical form of cysts present in dogs with GRPU. Iridociliary cysts arise most commonly from the nasal (medial) section of iris/ciliary body in dogs with GRPU. Thus, in the dog’s left eye, the cysts typically are present from 7:00 to 11:00, and in the right eye from 1:00 to 5:00. There are no hard and fast rules here, however—while it is uncommon for free-floating iris cysts to accompany GRPU, it is not impossible. Rarely, iridociliary cysts in dogs with GRPU contain blood.
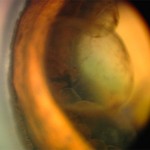
Left eye of dog NOT affected with GRPU (note normal light golden brown iris color); note semi-transparent iridociliary cysts arising at the 7:00 to 11:00 position from behind the brown iris, like ‘crowded tombstones’. Most of these cysts would not be visible unless the pupil was dilated. This dog is at risk for developing GRPU (Photo courtesy of Dr. Wendy Townsend)
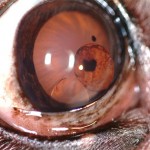
Right eye: Two large free-floating iris cysts in the anterior chamber of a dog with GRPU. Note their transparency. The dark brown dot above the right-hand cyst is a small cyst that ruptured and flattened out, its brown membrane sticking to the anterior lens capsule. This dog also has early immature cataracts. Note uniform dark brown iris hyperpigmentation. (Photo courtesy of Dr. John Sapienza)
Many of the iris cysts present in dogs with GRPU are not visible, especially if the pupils are not dilated with dilating drops at the time of examination. Additionally, it is impossible to see many of these cysts without the specialized equipment utilized by a veterinary ophthalmologist (slit lamp biomicroscopy). To further complicate matters, eyes enucleated from dogs with GRPU often demonstrate tiny iridociliary cysts microscopically but cysts are often not detectable clinically in these same eyes prior to enucleation. The cysts are often hidden from view behind the base of the iris, and often not visible clinically even after pupillary dilation. 1,3,4, 5
The relationship between iridociliary cysts and GRPU is not understood. Much more research is needed to help define the relationship (if any) between these two entities. It is unknown whether iris cysts cause GRPU, whether GRPU cause iris cysts, or whether iris cysts are unrelated entirely to GRPU. 2 As mentioned earlier, iris cysts in a Golden Retriever are a “red flag” and a risk factor for GRPU, and these dogs must be very carefully examined and regularly monitored by an ophthalmologist for the presence of GRPU.
GRPU is a pigmenting disease. This means that dark brown microscopic flecks of pigment are free-floating, like dust in the air, inside the anterior chamber and end up sticking to surfaces inside the eye, especially the anterior lens capsule. The pigment can clog the drainage holes inside the eye (iridocorneal drainage angle) that allow aqueous humor to exit the eye into the body’s blood circulatory system. One theory is that iris cysts cause glaucoma, 5 and another theory is that complex auto-immune mechanisms trigger pigment dispersion inside the eye and cause glaucoma. 4
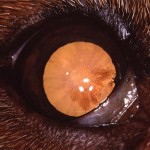
Right eye of dog with GRPU. Note streaks and clumps of pigment stippling the anterior lens capsule. Early immature cataracts are also present. Note uniform dark brown iris hyperpigmentation. (Photo courtesy of Dr. John Sapienza)
In fact, the signature clinical sign of GRPU is pigment deposits on the anterior lens capsule (ALC) ; the deposits are often “spoke-like” (“radial”), but can also be in clumps, especially on the nasal region of the ALC if iridociliary cysts are present; some of these cysts can rupture, causing the pigment from their brown membranes to adhere to the ALC. 1
Additional clinical signs that can be present (and usually are bilateral):
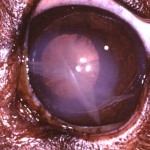
Left eye of dog with GRPU. Note cloudiness over pupil, with grey-white streaks. This is a ‘cloud’ of fibrin in the anterior chamber, centering over the pupil space. Note uniform dark brown iris hyperpigmentation. This eye also has late immature cataracts, and the conjunctiva is inflamed. (Photo courtesy of Dr. John Sapienza)
Cloudiness of the eye, associated with cataract—incipient or immature cataracts. It is rare for the lens to develop a mature cataract and blind the eye, but cataracts can certainly help impair vision. It is NOT recommended to perform cataract surgery on dogs with GRPU, as postoperative inflammation is severe and usually cannot be adequately controlled, leading to glaucoma and blindness. Present in the middle to late stages of the disease.
Bleeding inside the eye (hyphema). Sometimes it is more obvious that blood is inside the eye, than #5 (fibrinous plaque). When blood is present inside the eye, it is always accompanied by fibrinous material. Present in the middle to late stages of the disease.
Iris cysts. Usually nasal attached iridociliary cysts, but can be free-floating cysts in the anterior chamber. Present in the early stage of the disease.
Secondary glaucoma in the late stage of the disease.
Blindness in the late stage of the disease (due to glaucoma).
GRPU is a disease with a spectrum of clinical signs, and not all dogs with GRPU will have all of these clinical signs.
It is obvious from this discussion that GRPU is a complex disease with no firm understanding regarding genetics. Additionally, one study (Esson et al) has theorized that uveitis is not present in GRPU, based on histopathologic evaluation of eyes enucleated due to glaucoma. 4 However, other authors believe that uveitis is indeed present, and that the eyes from the Esson study showed little evidence of uveitis because the eyes had been treated with anti-inflammatory medication prior to their removal. It is Dr. McCalla’s opinion that because dogs with GRPU clinically respond favorably to anti-inflammatory medication, this is indirect evidence that inflammation is a component of the disease. It is obvious that in order to better understand GRPU, longterm studies of large numbers of dogs affected with GRPU are necessary. 2 There is no ‘best’ treatment regimen; all treatment regimens used by veterinary ophthalmologists are based on their personal clinical experience with the disease and not on research findings. This has evolved out of necessity, due to the lack of research regarding therapy of GRPU.
Treatment of GRPU depends on the stage of disease. It is the author’s opinion that if affected dogs are identified in the early stage of the disease and placed on lifetime treatment and examined regularly by an ophthalmologist, they will not progress to the middle and late stages of the disease and their vision is saved.
Dogs in all stages of the disease may benefit from lifetime supplementation with the canine antioxidant vision supplement, Ocu-GLO™ . An intriguing clinical study of dogs with GRPU supplemented with Ocu-GLO™ is currently being conducted by Dr. Wendy Townsend at Purdue University to determine if supplementation would be beneficial. This research was prompted by Dr. Townsend’s observation of one affected dog (that lost one eye to GRPU) undergoing spontaneous resolution of GRPU (i.e. resolution of pigment deposition on the ALC) in its remaining eye while on daily OcuGLO™ supplementation. Ocu-GLO™ also has been shown to be neuroprotective in the presence of glaucoma, and this nutraceutical may thus help preserve vision (and help preserve optic nerve function) in glaucomatous eyes.
In the early stage of GRPU, lifetime topical steroid and/or nonsteroidal anti-inflammatory medication is prescribed (the author prefers topical steroid medication, specifically prednisolone acetate 1% ophthalmic suspension) and the patients are reexamined every 6 months by the ophthalmologist. Owners are cautioned to contact the ophthalmology clinic if either eye has episodes of conjunctival redness or any signs of cloudiness. At each examination, tonometry is performed to monitor the intraocular pressures.
In middle to late stages, treatment is as for the early stage, but some dogs also need systemic anti-inflammatory medication. Many dogs respond with an oral non-steroidal anti-inflammatory drug (NSAID), but some dogs need an oral steroid instead.
Late stage cases usually have glaucoma or IOPs that are starting to elevate. These dogs also need topical glaucoma medications. Unfortunately, dogs initially presented to an ophthalmologist in the late stages of the disease often end up losing their vision due to uncontrollable glaucoma, and almost always, late-stage cases have both eyes affected, doubling the tragedy of this disease.
Surgical treatment for blind glaucomatous eyes must be performed if glaucoma cannot be controlled medically, because these dogs are in constant discomfort (similar to a migraine headache) and the eye(s) are enlarging because of the increased internal pressure. Because Golden Retrievers are wonderful, uncomplaining dogs, they will not usually let their owners know that their glaucomatous eyes are bothering them.
Many dogs with end-stage GRPU blinded by glaucoma end up having both eyes removed. Other more cosmetic surgical choices are available that are discussed in the glaucoma article. However, dogs with GRPU should not have the intravitreal injection of gentamicin (pharmacologic ablation) procedure performed, because it would create additional uveitis and discomfort in these dogs.
If a dog with GRPU blinded by glaucoma had high uncontrollable IOP(s) and was not healthy enough to undergo surgery, a therapeutic dilemma occurs, and often these dogs end up being euthanized because their quality of life with unrelenting migraine headaches is unacceptable, which underscores the tragedy of this disease. It cannot be emphasized too often, that early detection and lifetime treatment is the key to saving the vision in affected dogs.
How can you help reduce the incidence of GRPU in Golden Retrievers?
Be aware of the danger of red/pink conjunctiva and the risk of GRPU being present if iris cysts are present.
If you have a dog with this clinical history, OR if you know that your dog has iris cysts, seek out a veterinary ophthalmologist to examine your dog. To locate a board-certified ophthalmologist, visit the acvo.org website.
If your dog has GRPU, PLEASE treat your dog as directed by the ophthalmologist and bring it in as often as directed by the ophthalmologist.
Tragically, dogs have had their eyes removed, or been euthanized, because owners failed to follow directions.
If your dog has GRPU, inform your dog’s breeder of this diagnosis, so that the breeder can make knowledgeable decisions about their dogs.
Support Dr. Wendy Townsend’s GRPU research by donating funds (tax-deductible!) for her research, perhaps in honor of that special Golden Retriever in your life. She is the only ophthalmologist performing research on this disease. Here’s how you can help:
It is critical for the general veterinary practitioner to be aware of GRPU as a disease, and to refer suspected cases to an ophthalmologist ASAP.
GRPU is a very serious disease, in which early detection is critical—with early detection, dogs can be placed on lifetime anti-inflammatory medications and a special canine antioxidant vision supplement ( OcuGLO™—see www.OcuGLO.com ) to help control inflammation and also to help support the health of all the cells of the eyes, and the immune system too. Some severely affected dogs also need lifetime systemic medication (oral) to help control inflammation, and/or glaucoma medication to attempt to control glaucoma. If GRU is caught early enough, and if the dog is treated as prescribed by the ophthalmologist and is examined as often as needed by the ophthalmologist, vision is almost always saved.
And finally—If a dog loses their vision from GRPU, it is important to understand that they can still have a very acceptable quality of life without their sight, as long as they are not in pain. A blind dog is not suffering, as long as the eyes are comfortable. If they are uncomfortable (i.e. migraine headache from glaucoma) and this cannot be controlled medically, then surgery (such as eye removal) must be done. Their general health needs to be acceptable in order to perform surgery, and it is helpful if their environment is stable (don’t move furniture around in your home) and it also helps (but is not necessary) if they can still hear.
It is relatively rare for my patients blinded by GRPU to be euthanized; I have had many GRPU patients presented in the late stage of the disease, in which both eyes were removed. These dogs have always thrived postoperatively. A dog’s job is to be with their family and share their life with their family, and as long as that happens, they are happy!

This is “Chase” with a favorite toy—the same dog as shown in the beginning of this article. GRPU robbed this kind and gentle dog of his vision. He developed secondary glaucoma in both eyes, and both eyes were removed. Chase went on to live a full life, and even with no sight, he continued catching tennis balls!